Medics, Health Authorities and Patients: Keys in mitigating deaths from Non-Communicable Diseases
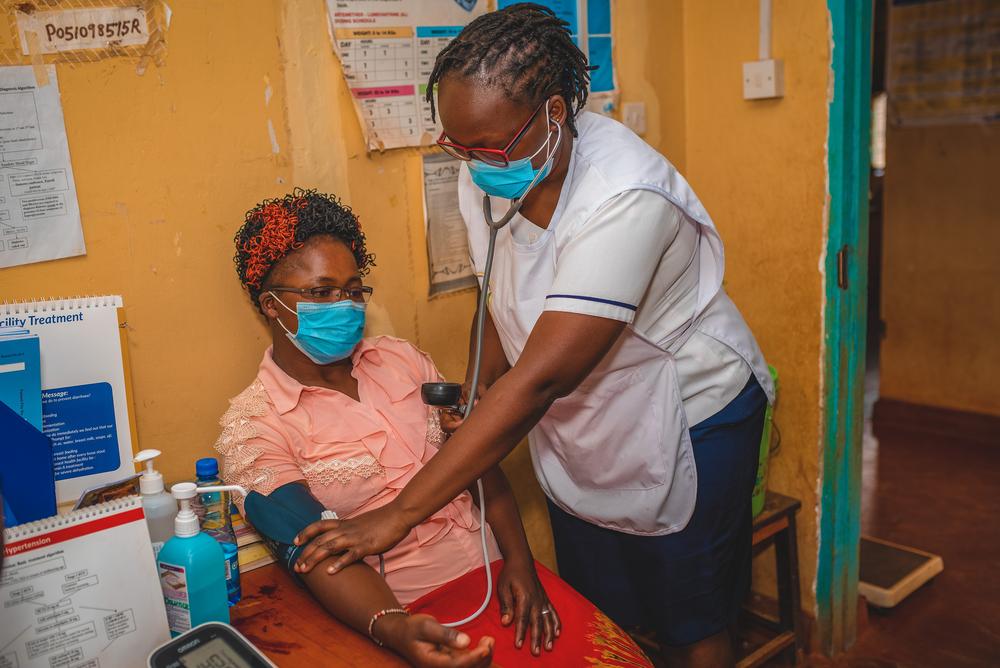
One on one session at Kabuguria Dispensary. Kenya, August 2021. © Nduati Mambo
Non-communicable diseases (NCDs) are the leading cause of death globally. According to the World Health Organisation, NCDs kill 41 million people each year, equivalent to 71 percent of all deaths globally. Each year, more than 15 million people between the ages of 30 and 69 years die from NCDs; 85 percent of these "premature" deaths occur in low- and middle-income countries.
In Kenya, NCDs account for 27 percent of the total deaths and over 50 percent of total hospital admissions.
For many years, patients with non-communicable diseases (NCDs) could only access services in the apex hospital of the county in rural Embu County in Central Kenya. This meant that many had to endure long and costly journeys to the main referral hospital, which was also in itself congested due to the high number of patients having to be seen.
In 2017, Doctors Without Borders started a program in Embu. The aim was to mentor, integrate and decentralize medical care for patients living with NCDs into primary health facilities, that is, the dispensaries and health centres, which are the lowest medical facilities in the cascade. In this response, Doctors Without Borders developed a model of care for NCDs that is effective to implement at Primary Health Care level. The model is also duplicable by Doctors Without Borders and the Ministry of Health (MoH). It was taught to MoH medical staff and Community Health Volunteers through a clinical mentoring, hands on training approach.

In addition to clinical mentoring, creating prevention awareness, Doctors Without Borders focused on managing and treating six NCDs conditions namely hypertension, diabetes, asthma, chronic obstructive pulmonary disease, epilepsy and mental health.
In June 2021, Doctors Without Borders handed over the NCD program to Embu County’s Department of Health, a process expected to be fully completed by December 2021.
The project findings are detailed in the first ever nationwide NCDs report.