About Doctors Without Borders
Doctors Without Borders / Médecins Sans Frontières (MSF) is an international medical humanitarian organisation. We deliver life-saving emergency medical humanitarian aid to people affected by armed conflict, epidemics, pandemics, natural disasters and healthcare exclusion.
We work in over 70 countries worldwide, from North Africa to South America, Asia Pacific and the Middle East, in villages not found on any map, in refugee camps, in hospitals and clinics, in projects, serving the health needs of the vulnerable.
Patients first
Our patients are at the core of our mission and our operations. We work to alleviate human suffering, especially in crisis situations, to protect life and health.
Doctors Without Borders field workers provide medical care to help people survive catastrophic situations, where communities and health structures may be overwhelmed. Where applicable, we also have MSF field research projects. In many places where we work, there are no other healthcare providers or aid organisations in the field. In other places, we work closely with the local ministry of health or other partners to ensure the best care for our patients.
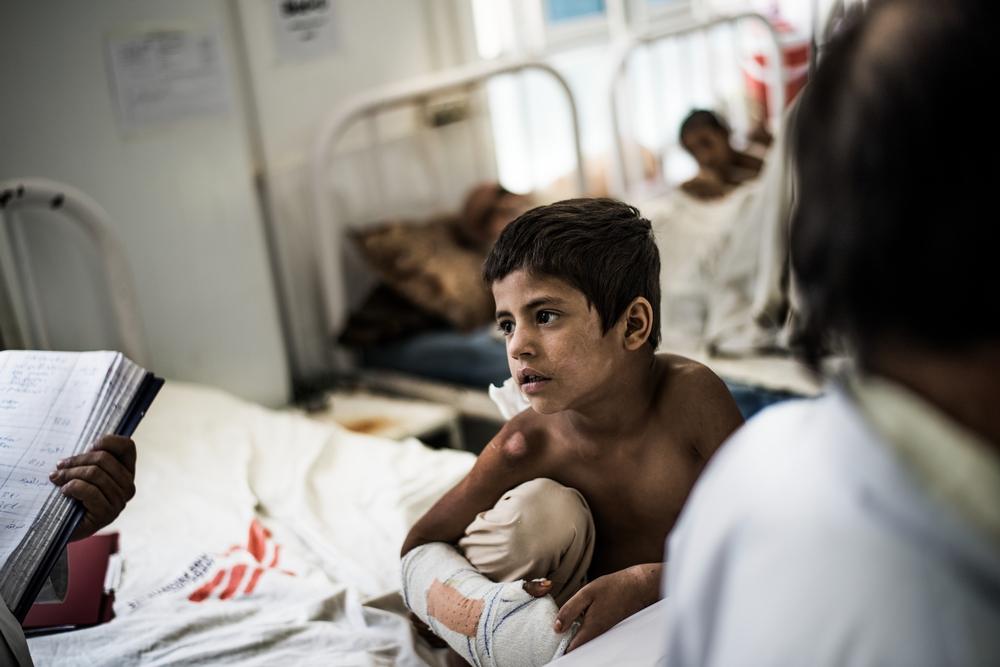
A child sits in the orthopaedic ward of Boost hospital which is run by Doctors Without Borders in partnership with the Ministry of Public Health in Lashkar Gah, Helmand, Afghanistan. © Kadir Van Lohuizen/Noor
Our history
Doctors Without Borders was founded in 1971 in France by a group of doctors and journalists in the wake of war and famine in Biafra, Nigeria. The aim was to establish an independent organisation that focuses on delivering emergency medical aid in the field – quickly, effectively and impartially.
Three hundred volunteers made up the organisation when it was founded: doctors, nurses and other staff, including the 13 founding doctors and journalists.
Doctors Without Borders was created in the belief that all people should have access to healthcare regardless of gender, race, religion, creed or political affiliation, and that medical needs outweigh respect for national boundaries. The principles of action of Doctors Without Bordersare described in our charter, which established a framework for our mission and our activities around the world.
What we do
The mission of Doctors Without Borders is to provide quality medical care to all our patients, despite challenging settings and limited resources in the field.
Our medical teams and field workers offer basic healthcare, performs surgery, fights epidemics, rehabilitates and manages hospitals and clinics, carries out vaccination campaigns, operates nutrition centres, provides mental healthcare and human resources, and offers training to local medical staff. Sometimes our work requires we build some form of water processing facilities, or support power supplies. Other times our projects offer the opportunity to build an MSF field research unit and publish our findings. Our emergency staff are trained and equipped with everything they need to bring rapid assistance to people in crisis.
With international staff and locally hired employees, we also provide medical care and psychological support to those living in chronic emergency situations, such as people displaced by conflict, epidemics or disaster. Our programmes treat patients with infectious diseases such as tuberculosis, HIV/AIDS and kala azar.
When needed, we construct wells, supply safe drinking water, and distribute shelter materials and other relief items such as cooking and washing kits.
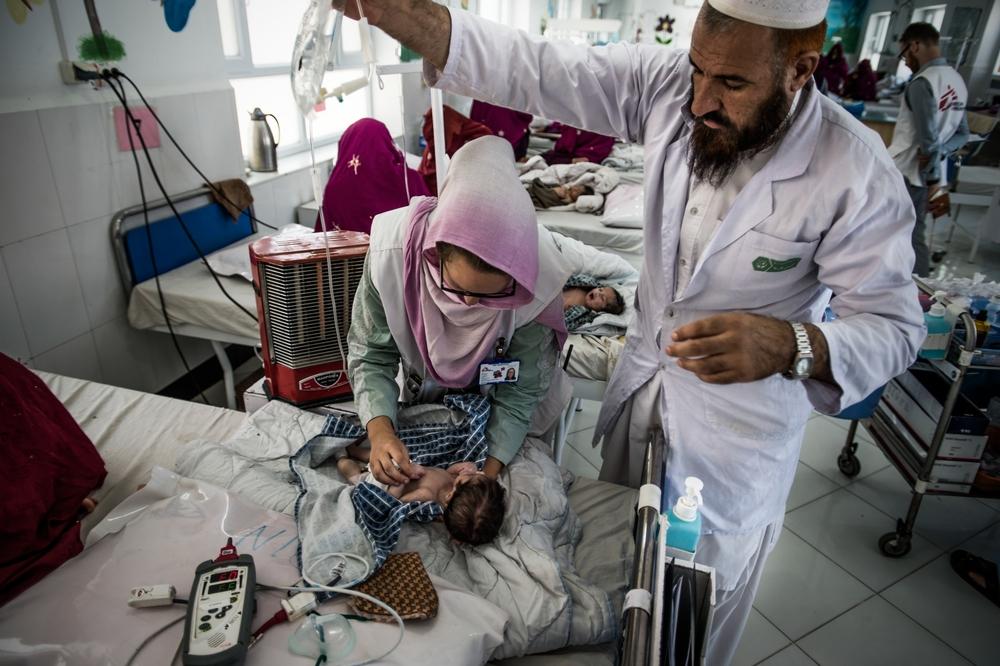
Doctors Without Borders nurse, Samantha Hardeman, at the neonatal intensive care of Boost hospital in Afghanistan. © Kadir Van Lohuizen/Noor
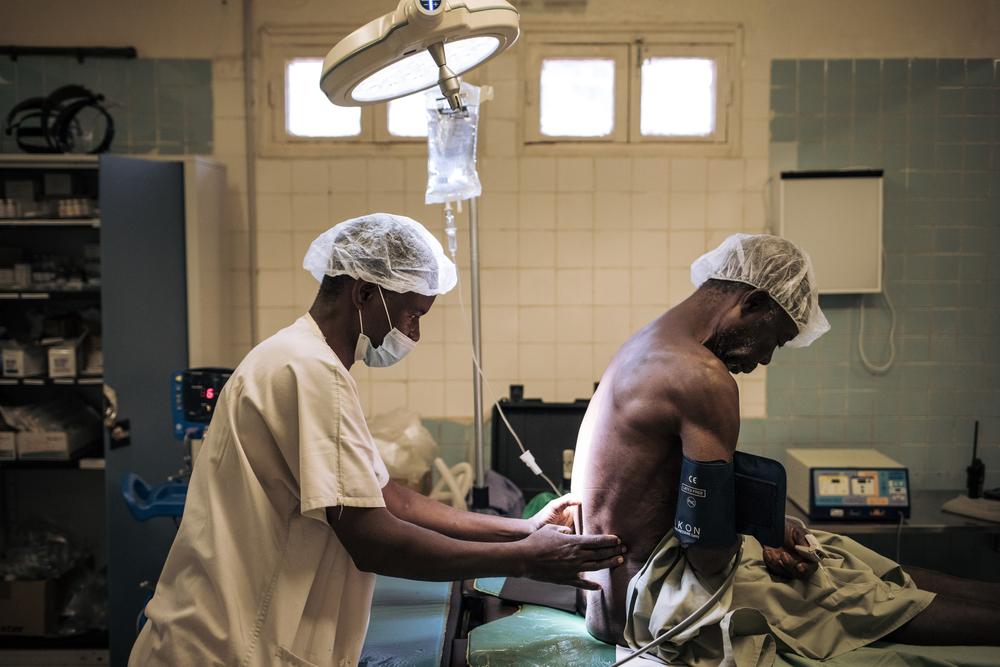
In Bangassou, Central African Republic, the Doctors Without Borders surgery team is operating a patient who suffers from inguino-scrotal hernia on January 2021. © Alexis Huguet/MSF
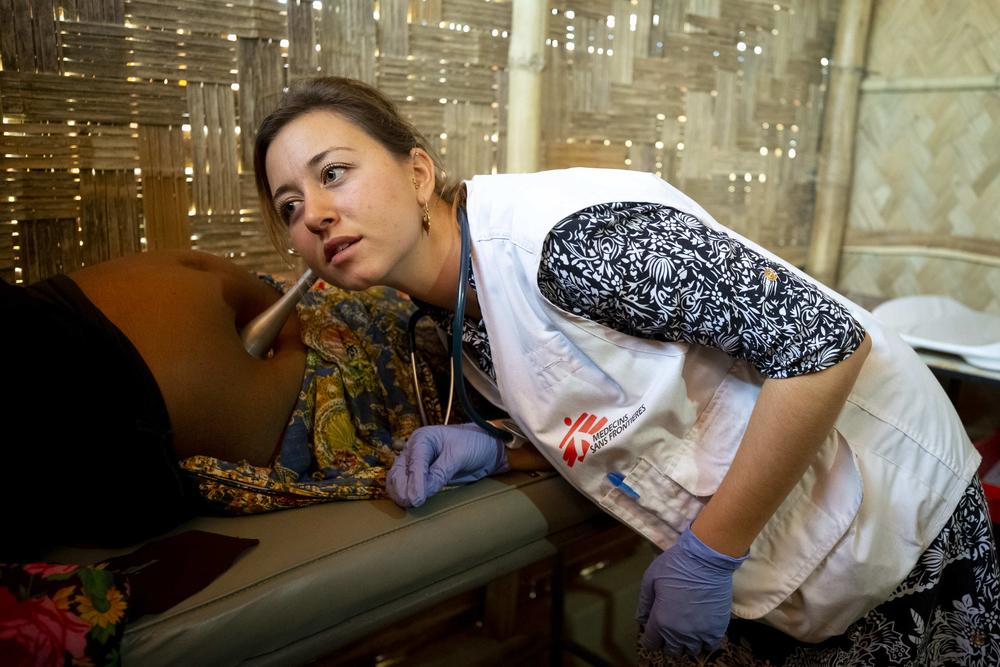
Laura, Doctors Without Borders midwife, checks the belly of a pregnant patient in Jamtoli camp, Bangaladesh. © Vincenzo Livieri/MSF

The Doctors Without Borders team visited one of the survivors in an evacuation camp at Susukan Kampong, Sukarame Village, Indonesia. Here they met a 13-year-old adolescent who is also a beneficiary of the MSF adolescent health project in Banten. © Muhamad Suryandi/MSF
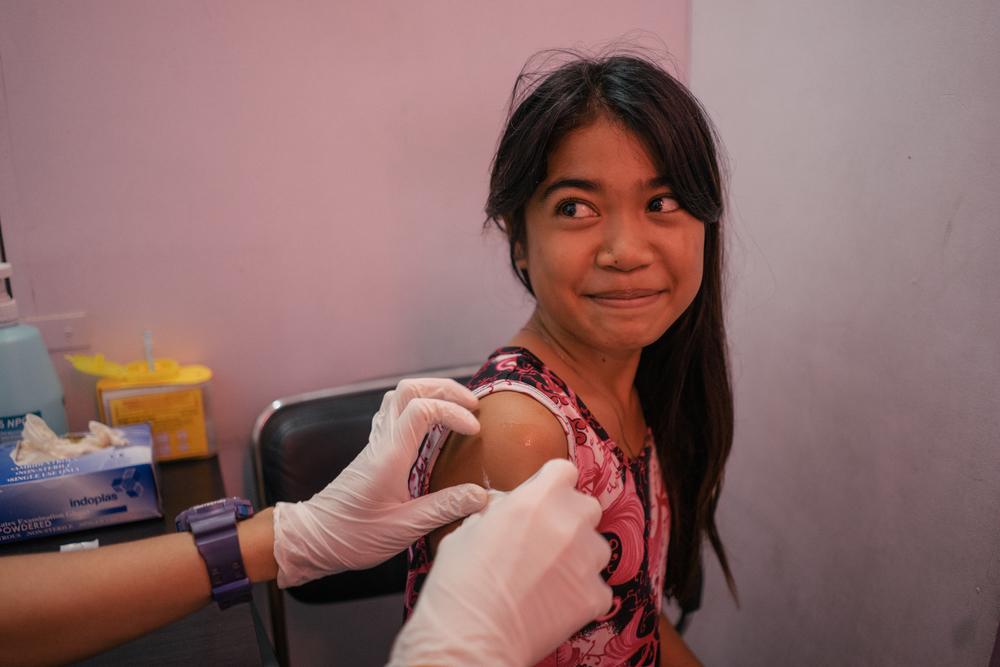
A young girl from Tondo, Manila, is seen in a Likhaan clinic for her free HPV vaccination. Likhaan provides reproductive healthcare services for low income families in the Philippines, where there remains a gap in women's awareness of their reproductive rights. © Hannah Reyes Morales
We act fast
Around the world, Doctors Without Borders teams are often the first in the field, particularly during disasters and crisis settings. Each region has its own logistics centre ready to supply equipment, medicine and other necessities. Field teams on assessment missions usually arrive first to determine the kinds of supply, medical knowledge and equipment required. The people we help usually have varying health concerns: mental health, trauma, dehydration, malnutrition, disease.
During the early months of the Ebola outbreak in West Africa in 2014, in many areas we provided the only medical care, and was the leading voice demanding the world’s attention.
After the devastating Haiti earthquake of 2010, one of our field teams treated the first survivors within minutes.
Disasters often affect multiple countries, such as African nations that share borders, Middle Eastern countries in conflict, and Southeast Asian countries hit by tsunamis and supertyphoons. In many such situations, every year, we provide aid in places one cannot even find on a map.

Maila Gurung, 26, is assisted off of a helicopter by MSF Dr. Hanni when returned home to Diol village, Gorkha District, Nepal on May 2015. Maila had been evacuated to the Doctors Without Borders hospital in Arughat Bazaar where his broken leg was treated. © Brian Sokol/Panos Pictures
- Stories from the field: Working in the mobile clinic
This triple disaster was Indonesian medical doctor Achmad Yusuf Toba’s first time to work with Doctors Without Borders. He talks about his field experience:
“When I learned that they were looking for medical doctors to respond to the tragedy, I immediately volunteered myself. When I arrived in the field, I learned that we had been providing medical care for the victims of the disasters in Palu and Donggala. They have been doing it since day two of their arrival in the region. My primary duty is to treat patients using the mobile clinic. My work mostly involved trauma patients, such as the case of a woman who got burned by boiling water as she was running out of her house during the earthquake. I also saw many patients who suffered from fractures (broken bones), and wounds of different severity – from bruises, lacerations and injuries. Part of what I did was to also assess the evacuation centres or health posts that the team set up, and to do disease surveillance and individual follow-ups of patients to ensure that communicable diseases like diarrhoea, skin problems and respiratory tract infections would be prevented.”
- Patient stories: Elis and Purwanto
Elis and her family were at home when the tsunami hit the coast of Sunda Strait on that fateful day. Their home was located on the shorelines of Laba Kampong, Cigondang Village, Labuan Sub-district. They lived just next door to the home of her parents.
When the first wave hit, Elis’ husband, Purwanto shouted a warning to Elis, and rushed to their daughter and his in-laws, who were next door, so they could seek safety.
The strong wave, taller than a nearby power pole and about 7 to 12 meters high, destroyed their house and reduced it to rubble. Purwanto, 35 years old, got injured when his left thigh was hit by the tin roof of their house. Elis was trapped inside the house by a cupboard and desk, and the rubble that was left of their home.
Fortunately, even injured, Purwanto was able to save Elis. Elis and Purwanto walked 2 kilometers towards the health centre in Labuan.
Elis and her husband were treated by the Doctors Without Borders team at the Labuan health centre. “They checked my condition and that of the baby. I had bruises with some swelling almost all over my body. But thank God, my baby is okay.”
The team attended to Elis and ensured her medical care. She stayed at the Labuan Health Centre for the next three days. Meanwhile, they referred Purwanto and Elis’ mother to the hospital in Pandeglang as their injuries were quite severe. Her father was also referred to the same hospital due to an injury on his left hand.
Supporting Indonesia amidst multiple disasters
On the 28th of September, 2018, a series of strong earthquakes struck Indonesia’s Central Sulawesi. The earthquake triggered tsunami waves, and the tsunami in turn caused landslides and liquefaction that swallowed entire villages. In all, the triple disaster killed 4,340 people.
The first Doctors Without Borders team that arrived in the field included a coordinator, a nurse, and a psychologist, as well as three nephrologists. A second field team of three staff with experience in natural disasters headed to Indonesia from Panama the same day. More surgeons, nurses, logisticians, and even a psychologist joined the mission. Relief material and medical equipment were also flown to Indonesia from Brussels and Bordeaux.
On the 22nd of December in the same year, a large portion of the southern flank of the Anak Krakatau volcano slid into the ocean, causing a tsunami that swept across Indonesia's islands of Sumatra and Java. By 28 December, the Indonesian National Disaster Management Agency (BNPB) reported that there were 40,386 people displaced, with more than 80 percent of those displaced coming from Pandeglang District in Banten Province. The death toll increased to 426, with 7,202 injured, 23 people missing, and 1,296 houses damaged.
We mobilised three teams: one team supporting the Carita Health Center, and the second team supporting the Labuan Health Center. In both centres, we provided assistance to the health personnel attending to the injured in the field. A third team was mobile, visiting the various communities to treat injured patients who could not go to the hospitals or health centres. Case management was done on the go, with severe cases being referred to hospitals.
In the health centres, we provided medical care and ensured that Infection Prevention and Control protocols were in place. The team has also initiated the provision of Psychological First Aid (PFA) among admitted patients, and launched a mental health programme.

During our Typhoon Haiyan response, the mobile team consisting of a medical doctor, nurses, a psychologist and a logistician travelled by boat to remote coastal villages which could not be reached by road and had yet to receive any medical and humanitarian aid. © Florian Lems/MSF
- Stories from the field: Logistical challenges in emergency aid
Ten days after the typhoon struck, Emergency Coordinator Caroline Seguin described the huge logistical and human resources challenges of getting emergency aid and supply to where it was needed most.
“In the days since the typhoon hit, we’ve managed to bring more than 150 staff and hundreds of tonnes of supplies into the country. With so many health facilities damaged or destroyed, the healthcare needs are significant, especially since the living conditions exacerbate the risk of respiratory tract infections, pneumonia and waterborne diseases. In most areas where are working – Panay, Guiuan, Ormoc, Tacloban and Burauen – the health services have been severely disrupted and we’re focusing on restoring quality primary healthcare and hospital services. In Guiuan, a tent hospital has been put in place in the premises of the damaged reference hospital, while in Tacloban, an inflatable hospital will be set up this week and will provide all services including emergency room, inpatient department, and operating theatre. Teams will urgently set up maternity, obstetrics and gynaecology units. In such an apocalyptic situation, the need for mental health services is overwhelming. All of our teams include mental health officers or psychologists. It’s an extremely important aspect of our response, and quite straightforward to implement compared with other more logistically challenging services."
Medical teams arrive in the Philippines one day after Typhoon Haiyan
In 2013, Typhoon Haiyan – one of the strongest super typhoons ever recorded – caused over 6,300 confirmed deaths and displaced four million people in the Philippines. Essential infrastructure, including health facilities, roads and ports, were damaged or destroyed, and emergency supplies swept away. The medical needs were immense, and the risk for communicable disease outbreaks was high.
Doctors Without Borders was able to dispatch teams to the affected areas within a day of the super typhoon making landfall.
Primary relief activities in the aftermath of Haiyan included 11,624 surgical interventions; 29,188 vaccinations for tetanus, measles, polio and hepatitis; mental health care and/or counselling for 27,044 patients; 2,445 babies delivered; mobile clinics in 133 different locations; the construction of one semi-permanent hospital; the rehabilitation of seven hospitals; supply and distribution of 71,979 relief kits; food packs for 50,000 people; and distribution of 14,473,500 litres of water.
In total, we 1,855 tonnes of cargo and deployed almost 800 relief workers to the Philippines at the height of our response. This large-scale field action was enabled by the generosity and compassion of individual donors and supporters worldwide. Internationally, we raised a total of 32.4 million euros in funds for the Typhoon Haiyan response.
We treat the vulnerable
Every year, as an international medical humanitarian organisation, the Doctors Without Borders / Médecins Sans Frontières (MSF) mission includes providing medical aid in refugee camps and detention centres around the world. In Southeast Asia, we have been working to provide healthcare to the Rohingya, one of the most persecuted minority groups in the world.
Following a concerted campaign of extreme violence by the Myanmar authorities against Rohingya people in Myanmar’s Rakhine state in August 2017, over 700,000 Rohingya fled over the border into the Cox's Bazar district of Bangladesh.

Um Kalsoum lost two children in the August 2017 killings in her village in Myanmar. Her 18-month-old boy Abdul Hafiz survived. © Mohammad Ghannam/MSF
- Stories from the field: Left to starve at sea
Loaded like human cargo into a wooden fishing trawler, around 500 people attempting to reach Malaysia from refugee camps in Bangladesh were starved and beaten by smugglers during a two-month voyage in 2020. All of the passengers were ethnic Rohingya from Myanmar, and most were aged between 12 and 20 though there were also some young children. Denied permission to land in Malaysia, the 400 or so survivors were eventually rescued by the Bangladeshi coastguard.
Amina*, a 14-year-old Rohingya girl from a small market town in western Myanmar, describes sitting on deck under the burning sun with hundreds of people for over two months. “We had to sit like this,” she says, hugging her knees to her chest. “People’s legs swelled and got paralysed. Some died and were thrown into the sea. We were adrift at sea with people dying every day. We feel like we’ve been taken from hell."
The refugees say they were beaten at the slightest provocation and given minimal food and water. “It was extremely hot and there was no food, no water,” says Amina. “We got one handful of dal and one capful of water per day.” Other survivors say they often received no food or water at all for days at a time. Desperately thirsty, many people resorted to drinking seawater.
The boat was denied permission to land in Malaysia, or in any other location, and eventually turned back towards Bangladesh. Some days before reaching Bangladesh, most of the smugglers abandoned the boat and its starving passengers. The Bangladeshi coastguard rescued the 400 or so remaining survivors. We sent teams of medical and mental health staff to support the rescue and provide emergency care to the emaciated survivors as they arrived back in Bangladesh. Medics stabilised those who were acutely unwell and referred some to MSF hospitals for malnutrition with severe complications and other conditions. Our mental health teams provided counselling to the survivors.
“Mostly people were stressed and really traumatised, frightened, uncertain. They were grieving for lost family members, and there were children who had lost their parents,” says Hanadi Katerji, nurse and medical team leader.
“The boat crew told us: ‘Everywhere you’re a refugee,’” says Amina. “In Myanmar you’re a refugee, in Bangladesh you’re a refugee, in the boat and in Malaysia too you’re considered a refugee. You will die wherever you go.”
We respond to health crises
Doctors Without Borders started responding to the Ebola outbreak in 2014, and continued working on multiple outbreaks. But there are other pandemics and epidemics. Outbreaks of cholera, measles and yellow fever can spread rapidly and be fatal. Malaria is endemic in more than 100 countries. Millions are living with HIV/AIDS and tuberculosis.
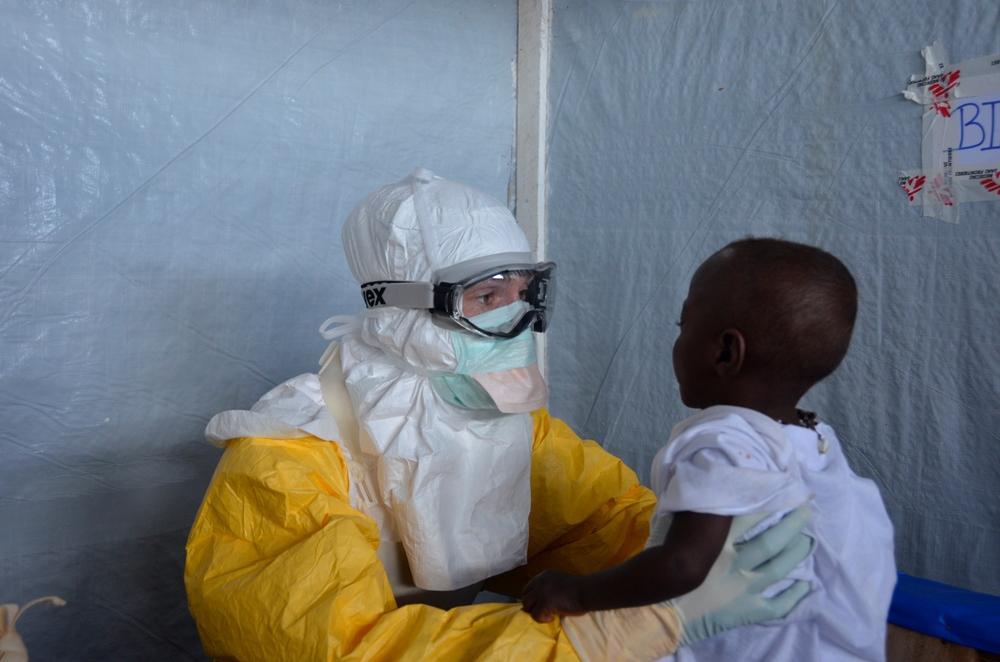
There are many children in the Guéckédou Ebola case management centre in Guinea, West Africa. Some are orphans, which makes caring for them more complex. Staff easily become attached to these patients, whom they are the only ones to touch and comfort through two pairs of gloves and a mask. © Julien Rey/MSF
Now, COVID-19 has affected virtually every country and region on earth, infecting tens of millions of people and resulting in the death of over a million more. In nearly every country, every region, every project, around Europe, Southeast Asia, Africa and the Middle East, we have supported COVID-19 response.
- Foreign domestic helpers in Hong Kong
In Hong Kong, we have been particularly concerned about public mental wellbeing during the coronavirus pandemic, especially amongst vulnerable groups who might have difficulty in seeking help. A survey showed that 72% of the foreign domestic helpers who responded have experienced depression-related symptoms. 47% in the survey sought help from their fellow workers in Hong Kong.
Doctors Without Borders/Médecins Sans Frontières (MSF) provided a training programme for community leaders in Hong Kong. By equipping them with the skills of active listening and psychological first aid, the aim was to empower them to better support their peers and understand their own boundaries when helping others.
Karen Lau, Doctors Without Borders/Médecins Sans Frontières (MSF) Mental Health Supervisor, said, “There are limited resources providing care for the mental health of Hong Kong’s foreign domestic helpers. However, we identified how their unique sense of community and extended peer networks can be leveraged to foster social support and improve their understanding of mental health. This can then allow foreign domestic helpers to better safeguard themselves and others amidst challenging times.”
We also conducted COVID-19 health education activities in Hong Kong, distributing leaflets in Tagalog and Bahasa Indonesia and other languages, organising learning sessions and answering questions. An emergency medical team reached out to vulnerable populations in Hong Kong: the elderly, street cleaners, the visually impaired, the homeless people, ethnic minorities, migrants and asylum seekers. In addition to sharing health education information, a special question and answer session was allotted to respond to the most immediate concerns.
- Community leaders in Indonesia
Early in the coronavirus pandemic, panic began to spread through Indonesian communities as COVID-19 cases were reported by health authorities. Rumours, myths and fake news proliferated. Community leaders and officials were bombarded by questions from community members pleading for clear facts about COVID-19. There was too much information coming from too many sources – social media, chat groups, and news reports on TV, radio and in print. The situation intensified when Kalibata village, in Pancoran sub-district, was declared a COVID-19 red zone.
A Doctors Without Borders/Médecins Sans Frontières (MSF) team assessed the situation in Kalibata village. The team discovered that confusion and fear were widespread in South Jakarta and that it was difficult for most locals to find trusted COVID-19 information sources.
“We discovered that the local health centres, or Puskesmas, were eager for our support,” says Dr. Dirna Mayasari, deputy medical coordinator in Indonesia. The Puskesmas invited community leaders, religious leaders and those trained to train others to voice their concerns in a meeting.
“The community needed clear advice on how to protect themselves against COVID-19. But they also wanted to talk. All the information they were getting was just one-way communication,” says Mayasari. “They wanted an opportunity to ask questions, discuss their worries and clarify the best methods to guard against this new virus. They also wanted to share ways to spread information within their communities.” Therefore, we decided to bring information closer and started conducting face-to-face trainings for the heads of the households that make up the community.
- Evacuees and urban poor in the Philippines
COVID-19 has proven to be a challenge to healthcare systems in all sorts of contexts, but it is even more difficult in places recovering from conflict, and in densely populated urban areas. Hygiene is a concern when access to clean water is limited. Infection prevention and control is an even bigger challenge when physical distancing is nearly impossible.
In 2017, an armed group laid siege to the city of Marawi in the southern part of the Philippines. Conflict erupted between the Philippine army and the group. The siege lasted five months and forced around 370,000 locals to flee their homes. More than three years later, around 70,000 people continue to live in harsh conditions in temporary shelters, and another 50,000 are estimated to be living in other family members’ houses. After the siege, Doctors Without Borders/Médecins Sans Frontières (MSF) field staff made sure evacuees had access to free and clean water. Later, the support extended to mental health care, and went on to include support for three health centers in the area, treating non-communicable diseases, such as hypertension and diabetes, and providing free medication.
When the COVID-19 pandemic started and community quarantine was imposed, medical consultations at health facilities were suspended. The lack of access to clean water made following the recommendations to contain the spread of the virus particularly challenging. Patients suffering from non-communicable diseases, such as hypertension or diabetes, were especially vulnerable to the virus. Teams carried out home visits to ensure patients continued to receive their medication and to provide patients with a leaflet about the virus and on how to protect themselves and their families from it.
In the capital city of Manila, the slums of Tondo are particularly crowded, making home isolation almost impossible. Because of movement restrictions and closed businesses, many were also out of work. To help those in home quarantine, our teams provided over 2,000 COVID-19 hygiene kits, the content of which included disposable masks, thermometer, alcohol, hand soap and the contact card of a social worker. The teams also provided hygiene kits for their contacts, with similar items in the content. Since those in quarantine could not work, we collaborated with a local faith-based congregation, the Missionaries of Charity, to provide food packs as needed.
Manila's San Lazaro Hospital initially had two COVID-19 Intensive Care Units that could cater for ten patients each. There was also one ward with 20 beds, one adult male ward housing 20 patient beds, and one adult female ward with 20 patient beds. We boosted SLH’s COVID-19 testing, data management, and COVID-19 case management capacities with biomedical equipment, medicines, medical supplies, personal protective equipment, and training for infection prevention and control.
We provided San Lazaro Hospital with human resources support, to assist at the Departments of Laboratory and Epidemiology, in the COVID-19 wards, COVID-19 triage and the Tuberculosis ward. In addition to staff, equipment and medicine, we also supported SLH with infrastructure improvement.
- Stories from the field: Religious observances during a pandemic
Chika Suefuji, project coordinator in Marawi, talks about the challenges the community faced when community quarantine was imposed in March 2020.
"People couldn’t go to their masjid or mosque, which is one of the most important practices during Ramadan. Some were understandably upset to learn that they had to observe Ramadan differently; some questioned this decision, since only a few cases of COVID-19 infections had been reported in the area. We discussed this with the community and religious leaders, explaining how the virus spreads. They understood well and put out a statement asking everyone to follow the safety measures. This approach helped to disseminate accurate information and convinced a larger number of residents to follow the measures. Overall, everyone have respected social orders to protect their families and communities, and it has helped contain the virus in the community.”
- Stories from the field: Food packs and psychological first aid to survive quarantine
Due to the difficult conditions brought about by the COVID-19 pandemic, many families in Tondo experienced anxiety and depression. Lyka Lucena worked as a mental health social worker, and she said, “They were worried about infecting others especially their loved ones. They were also scared of getting sick or getting COVID-19 again. A lot of patients were experiencing loneliness due to being away from their families. Many shared feelings of anger, frustration, and helplessness about their situation.”
Doctors Without Borders/Médecins Sans Frontières (MSF) teams offered remote mental health support to those in isolation at home. “We tried to help alleviate their distress by identifying and emphasising their healthy coping strategies and to establish ways of helping themselves. We also made sure to address feelings of being discriminated and stigmatised. We also encouraged patients to reconnect with their loved ones,” said Lucena.
- Migrants and refugees in Malaysia
Malaysia has a robust healthcare system, but COVID-19 shows that policies of social exclusion and limited access to health care can impact society as a whole. Though the government decided to ensure free access to Covid-19 testing for all, refugees and irregular migrants still live with a constant fear of being arrested and detained. This fear exists at home and in the street – as immigration raids are frequent- but even at health care facilities.
This is why we have been calling on the government to repeal Circular 10/ 2001, under which healthcare providers are obliged to report “illegal immigrants” (pendatang asing tanpa izin, or PATI) seeking healthcare services to the police and immigration authorities. We have also been calling for access to a subsidized health insurance and a legal status for irregular migrants in Malaysian law, which exempts them from the Immigration Act.
We are also advocating for the Malaysian government to cease targeting migrants and refugees in immigration raids, which risks further spread of COVID-19 in detention centres.
In addition to speaking out about the status of refugees and irregular migrants, in Penang we are providing COVID-19 health education in different languages, including Rohingya and Burmese, and translations in hospitals. We also conducted a COVID-19 health promotion campaign for Rohingya refugees via an online Rohingya news network.
We speak out
As Doctors Without Borders was founded by both journalists and doctors, we are not content to do medical humanitarian work. We feel that speaking out--what we call temoignage--is an important element of the work we do.
Temoignage is done with the intention of improving the situation for populations in danger. When we witness mass violations of human rights, for example genocide, war crimes, forced return of refugees, we may speak out publicly. Speaking out includes campaigning and lobbying for more equitable access to healthcare, such as years-long campaigns to lower prices for tuberculosis medication, and more recent campaigns to ensure that poorer countries will have enough supply of COVID-19 vaccines.
There are cases when it may be in the best interests of the victims for MSF to provide assistance without speaking out publicly or to denounce without providing assistance, for example when humanitarian aid is manipulated.
We believe it is important that we are honest about the difficulties of delivering medical aid under emergency situations, and we don't always get it right. Therefore, we continually reflect and seek to get better. We are committed to regularly evaluating the effects of our activities, and account for our actions to our patients and donors.
We are independent
Doctors Without Borders is a private international association. MSF associations are made up mainly of doctors and health sector workers and is also open to all other professions which might help in achieving its aims.
We rarely take funds from governments for our work, but rely mainly on the generosity of individual members of the public. Over 90 percent of our funds come from private donors giving small amounts. Our financial independence also means the aid we provide cannot be used to further any government's political or military goals.
We strive to ensure the evaluation of medical needs, and access to patients are without restrictions. This means that when there is an emergency, we can act fast by making use of funds from private donations to save lives, based on the independent assessment of needs.
Our approach does not always sit comfortably with the usual charity sector style. We never launch an emergency appeal unless we are certain we can spend the money on that specific crisis; there are no asterisks or hidden disclaimers diverting money to other parts of the organisation.
We’ve even offered money back when public generosity has outstripped the response, or else made sure our supporters were happy to have their money spent elsewhere. Except for emergency appeals, we ask that donors give to our general funds, contributing to an emergency reserve which is ready to use when a disaster strikes.
According to 2019 activity reports, more than 6.5 million individual donors and private institutions (private companies and foundations) provided 96.2 per cent of the €1.63 billion raised in funds.
Our funds rely largely on individuals donating small amounts. This helps to ensure our operational independence and flexibility to respond at a moment's notice to the most urgent crises, including those which are under-reported or neglected.
Since 2016, we refuse to take funds from the European Union, its Member States and Norway, in opposition to their damaging deterrence policies on migration and their intensifying attempts to push people away from European shores.
Moreover, we don't accept contributions from companies and industries whose core activities may be in direct conflict with, or limit our ability to provide medical humanitarian work. Hence, we don't accept money from: pharmaceutical and biotechnology companies; extraction industries (such as oil, natural gas, gold, or diamonds); tobacco companies; and arms manufacturers.
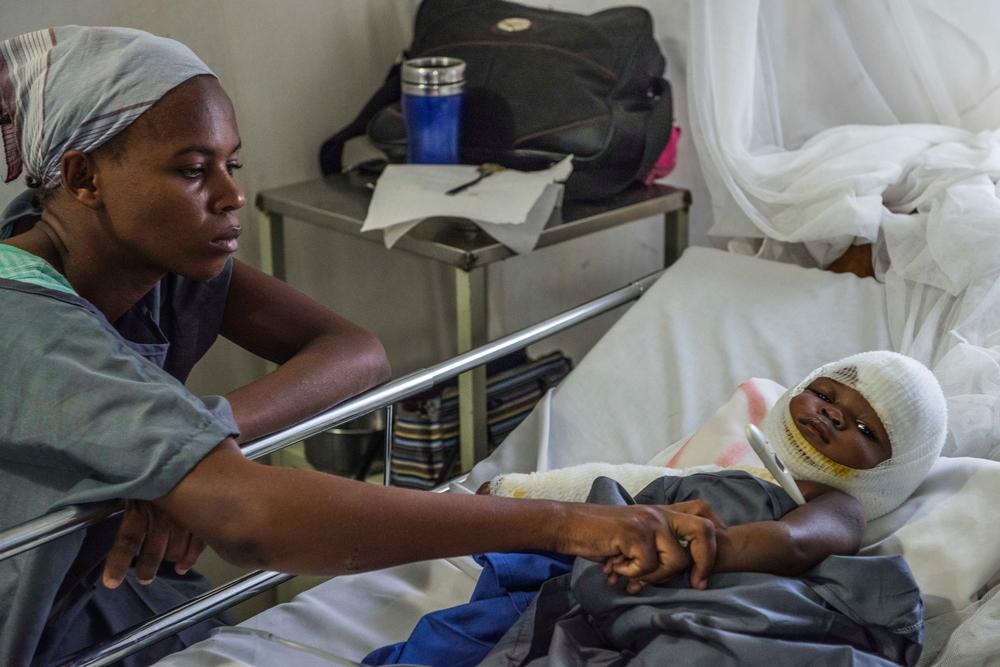
Severe burn victims in Doctors Without Borders Drouillard hospital in Haiti. © Yann Libessart/MSF

No safe haven for Iraq’s displaced. © Mohammad Ghannam/MSF

In our search and rescue operations in the Mediterranean Sea, these survivors were triaged by Doctors Without Borders medics and assisted by the Sea-Watch protection team upon embarkation. © Chris Grodotzki/Sea-Watch.org
We are neutral and impartial
We provide free medical care to those who need it the most. It doesn’t matter which country or region they are from, and regardless of their race, gender, as well as their political, economic or religious stances and interests. We give priority to those in the most serious and immediate danger.
We do not take sides nor support the agendas in armed conflicts, but go where the medical needs are greatest. Sometimes we are not present on all sides to the conflict; this may be because aid access is denied, or due to insecurity, or because the main needs of the population are already covered.
In a field hospital, it is not unusual that wounded civilians are alongside injured soldiers from opposing sides. Arms and weapons have to be left at the gate.
We treat our patients with dignity
Doctors Without Borders actions are first and foremost medical. We carry out our work with respect for the rules of medical ethics, in particular the duty to provide care without causing harm to individuals or groups. We respect patients' autonomy, confidentiality and right to informed consent. We treat our patients with dignity, and with respect for their cultural and religious beliefs. In accordance with these principles, we endeavour to provide high quality medical care to all patients.
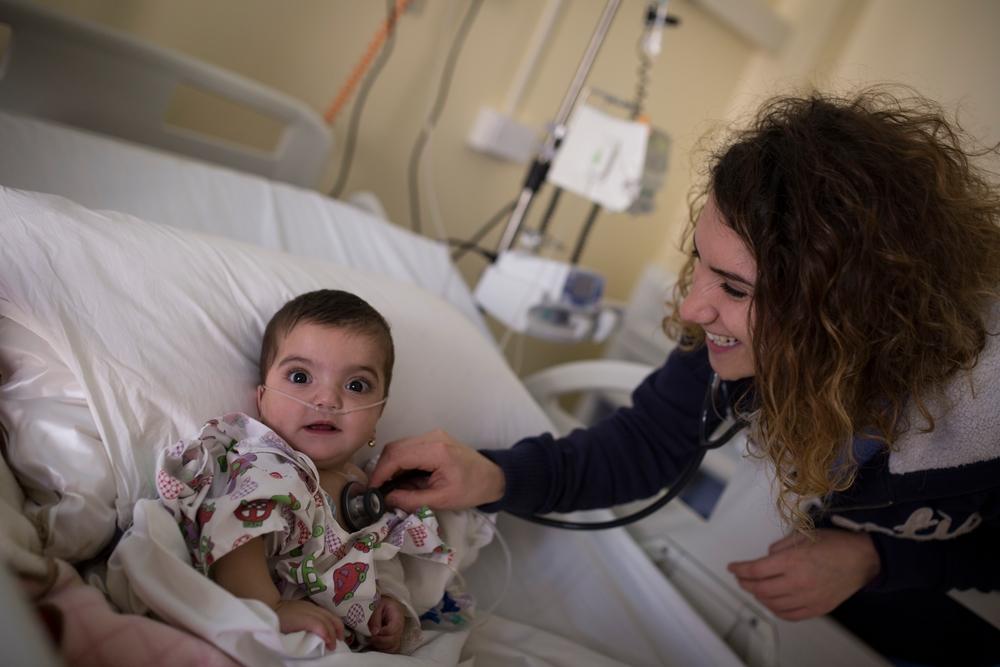
Pediatric services in Zahle hospital, Bekaa Valley, Lebanon. © Florian Seriex/MSF

Kids’ Zone at Doctors Without Borders Thalassemia programme in Lebanon. © Joffrey Monnier/MSF

Doctors Without Borders nurse Aiofe Ni Mhurchu' giving some anti-sea sickness pills to one of the 27 persons rescued in the Mediterranean Sea in January 2017. © Federico Scoppa