Afghanistan: Expanding access to urgently needed maternal health care

A midwife accompanies a pregnant woman in the labor room at the Doctors Withotu Borders Khost maternity hospital. Afghanistan, 2021. © Oriane Zerah
As an independent medical humanitarian organization, Doctors Without Borders relies mainly on private funding and so is not beholden to the political whims of governments. Our teams have been able to continue providing lifesaving medical care across the country, despite the difficulties we’ve faced accessing funds to pay staff salaries and cover operating costs. But we’ve witnessed critical funding cuts to the Afghan health system since the Taliban took power in August. This, on top of other economic measures taken against the new government, has contributed to a financial crisis that is severely affecting people all over the country.
Very quickly, we saw the capacity of the health system deteriorate. Public facilities had fewer and fewer drugs, as the supply chain was broken. Staff weren’t getting paid. We even heard that a local hospital was performing operations by flashlight. The public health system, which was already struggling before the suspension of funding, was barely functioning anymore.Lou Cormack, Project Coordinator
Although some funding has been released, the amount falls severely short—far below funding levels prior to the change of government—and is insufficient to improve a health care system that has failed to meet people’s needs for years.
Care by women for women
Doctors Without Borders opened the maternity hospital in Khost—the largest city in southeastern Afghanistan—in 2012 to provide safe and free sexual and reproductive health care to women and newborns, especially those who are at high risk of experiencing a complication during birth or after. In rural areas of Afghanistan, most women do not have adequate access to essential obstetrics care for many reasons, including the shortage of female midwives and doctors.
Ensuring a separation between men and women is essential in Khost maternity hospital, not only is it an important cultural practice in this area of Afghanistan but having women available to provide sexual and reproductive health care to women also creates a more comfortable and supportive environment for the patients.
The initial suspension of funding and now the cash crisis has made it even more difficult for women to access essential health care: Even when female midwives and doctors were available, they didn’t have the supplies they needed, and many health care workers have not been paid for months.
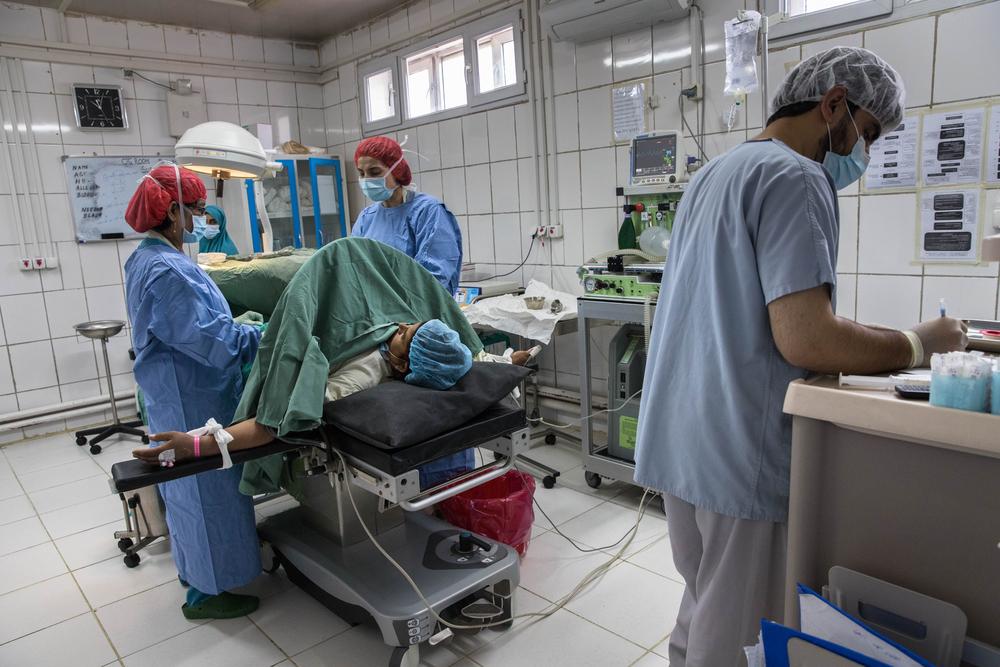
The operating theatre at the Doctors Without Borders Khost maternity hospital provides surgery to women who experience complications during pregnancy. Afghanistan, 2021. © Oriane Zerah
Despite the crisis, Doctors Without Borders has continued running all five of its programs across the country, including Khost, where Doctors Without Borders is one of the largest employers of women in the province. Doctors Without Borders' female Afghan staff are at the forefront of keeping the maternity hospital running, even during crisis. More than half of our 450 staff are female and hold a range of positions: doctors, midwives, nurses, cleaners, and carers.
During an uncertain time for Afghanistan, and as people face enormous barriers to accessing health care, Doctors Without Borders midwife, Aqila, said she finds great comfort in helping the women in her community. “I like to help the women who deliver in Khost,” she said. “The Doctors Without Borders maternity is a safe and great place for them. I delivered my own baby here. I love being a part of it. I really have a soft spot for mothers, because they suffer so much.”
Khost maternity hospital has a 60-bed inpatient department, an eight-bed delivery unit, a 28-bed newborn unit with a 10-bed neonatal intensive care unit, two operating theaters, and a dedicated kangaroo mother care area (in kangaroo care, mothers are encouraged to make skin-to-skin contact with their babies). We also provide vaccinations for newborn babies, family planning services, and conduct health promotion activities.
Thousands of births assisted
Following the change of government—which saw markets and transportation systems close, people too afraid to leave home, and many unsure if health facilities were still open— we decided to expand the admission criteria to assist all pregnant women, not just those at high risk for complications. Although some of these issues have now resolved, the funding crisis has continued to make it difficult for pregnant women to access the care they need to have a safe delivery.
In September, our team assisted nearly 1,650 deliveries—two months later, that number jumped to more than 2,000 deliveries in November. “We’ve had so many patients lately,” said Cormack. “We had 73 deliveries in one shift, and patient numbers have been increasing over the last few months. We know this is happening because public health facilities are closed, and private doctors are very costly. When women can’t afford to come for health care and give birth at home, they [face multiple risks] such as hemorrhage or high blood pressure disorders related to pregnancy, [and have] no one there to diagnose it.”
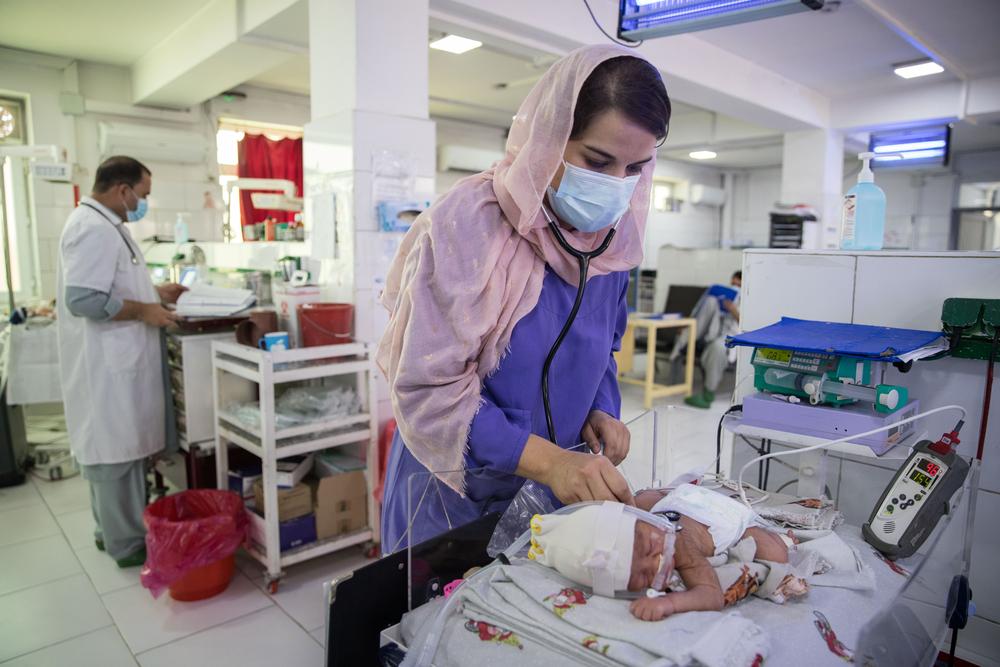
A pediatricians look after newly born babies in the neonatal ward at the Doctors Without Borders Khost maternity hospital. Afghanistan, 2021. © Oriane Zerah
Health care staff around the country have worked tirelessly to continue providing care to pregnant women despite funding being taken away from their facilities. “In the public system, we’ve heard of people pooling their money to buy medical items to keep their facilities open,” said Cormack. “If a woman needs a caesarean-section they all [contribute] to buy enough fuel so the generator can run during the procedure. This is despite the fact that health care workers and other civil servants haven’t been paid for months.”
Doctors Without Borders has also provided support to the delivery units in eight local primary care facilities in rural districts in Khost. Recently our teams have assisted with extra maintenance to make sure the facilities can keep running—for example, supplying fuel so that they can function at night, or kits for uncomplicated deliveries that include drugs, hygiene items, and a hat to keep the newborn warm.
The organization that runs many of the local health centers in Khost’s districts has now received funding until January—but it remains uncertain what will happen after that. Until these centers are fully functioning and used by the community again, our maternity hospital will continue providing care to all women who need it.





