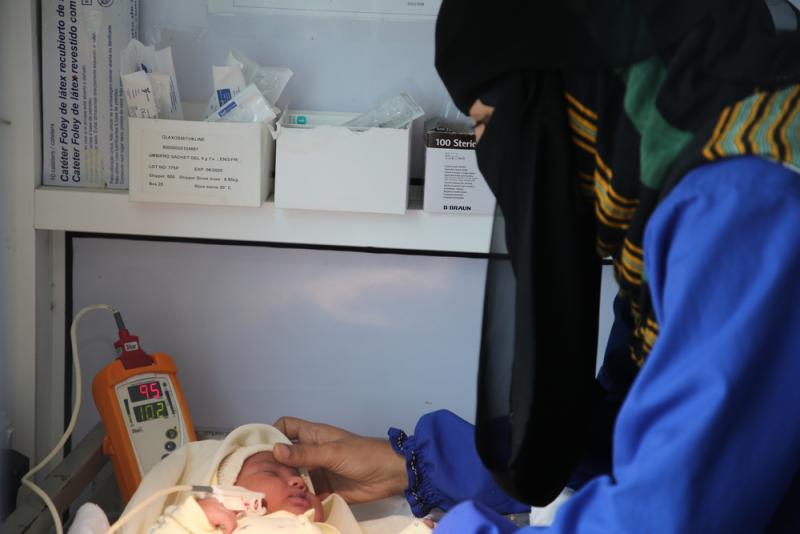
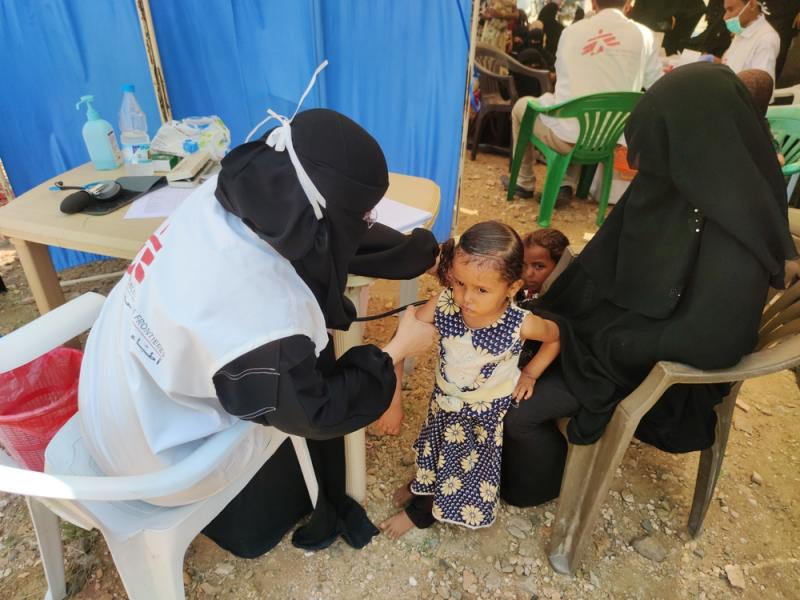
We deliver lifesaving medical care
Doctors Without Borders / Médecins Sans Frontières is a global medical humanitarian organisation that offers assistance to people based on need and irrespective of race, religion, gender or political affiliation. Since 1971, Doctors Without Borders has operated with a fierce—and challenging—commitment to independence, impartiality, and neutrality.
These principles make it possible for us to respond rapidly to emergencies and provide lifesaving medical care in situations where many other organisations can’t or won’t. This commitment ensures that we can help people in need as our singular purpose, rather than following other priorities—whether they be those of politicians, funders, or the media.
We chose to uphold a strict code of medical ethics during our work, ensuring we do no harm and put those most in need of medical care ahead of any other consideration. It is extremely important for Doctors Without Borders that our staff is in direct contact with the patients and with the communities for which we work.
Our work is not only to provide medical help but also an act of solidarity. We believe that these principles we stand for align with the principles of Islamic charity.
Subscribe to receive news and stories from our medical projects worldwide.

Help us support people caught in crises
Your donation helps us provide medical assistance to people caught in crises in Palestine, Yemen, Syria, Pakistan, among others.
Your donation to our humanitarian work respects Islamic principles of charity
Doctors Without Borders has been advised by a prominent Sharia Advisory Firm that ensures we can allocate your giving in accordance with our own medical humanitarian requirements and Islamic principles. To know more, please contact us by email at [email protected].
Doctors Without Borders has received donations and collaborated with Islamic Charity organizations, including prominent Zakat agencies. With the Guidelines provided by a prominent Sharia Advisory Firm and experience in collaboration with Islamic Philanthropy stakeholders, Doctors Without Borders is dedicated to establishing new partnerships and developing successful practices in implementing and processing Islamic Social Finance instruments/donations.
Doctors Without Borders accepts funds from corporations except those from excluded industries that derive a significant portion of their income from the production and/or sale of tobacco, alcohol, arms, pharmaceuticals (including: medicines, medical equipment, therapeutic foods, diagnostic and biotechnical materials, and research), and/or mineral, oil, gas, or other extractive industries. Please see the summary of our Gift Acceptance Policy.
How Doctors Without Borders use your donations
For every amount you donate, 80.5% goes directly towards providing lifesaving medical aid to people in need around the world, including those in Palestine, Yemen, Afghanistan, Syria, Somalia and on medical projects specific for the Rohingya. Only about 15.1% of donations received is reinvested in fundraising and 4.4% goes to management and general administration costs. Maintaining this standard is our priority to ensure that your contribution helps to relieve suffering and save lives in our various projects in over 70 countries worldwide.
In 2021, 55% of programme expenditure was spent in Africa, 20% was spent in the Middle East and North Africa, 11% in Asia and Pacific, and the rest in the Americas, Europe and Central Asia. We spent the most in the Democratic Republic of Congo, Yemen, South Sudan, Central African Republic, Nigeria, Sudan, Afghanistan, Ethiopia, Haiti and Niger. The International Financial Report gives more details of the geographic distribution of expenditure. It also provides breakdowns of expenses and funding for all the countries where Doctors Without Borders has significant programme activities in a given year.
The escalation of violence broke out in Gaza and Israel on 7 October. This has led to heavy Israeli bombardment and indiscriminate attacks, leaving thousands of people injured, and many killed. More than 2.2 million people are currently trapped in Gaza and grave humanitarian need.
Today, almost 85% of the Gazan population has been forcibly displaced by the Israeli forces. People are now living in rough conditions, with a lack of food, clean drinking water, shelters, health services and proper hygiene. And specifically, Rafah which has now become the most densely populated area in the Gaza Strip.
Doctors Without Borders is calling for an immediate and permanent ceasefire in Gaza now.

Powerful earthquakes hit the south of Türkiye and northwest Syria on 6 February, resulting in a shocking number of deaths and injuries, as well as massive damage to infrastructure.

The consequences of the earthquakes have exacerbated the already precarious humanitarian situation for people in northwest Syria. Both medical and relief support remain priorities to attend to the needs of thousands of people who lost their homes and are now exposed to extremely cold temperatures.
Our teams in northwest Syria are supporting medical facilities by providing staff and donations, supporting ambulances to facilitate the referral of patients, providing relief items to people affected, setting up mobile clinics in shelters and reception camps, and offering psychological aid.
People struggle to access medical care in Afghanistan. This is why we remain in the country, despite major attacks on our healthcare facilities and political uncertainties, to address people’s needs.
Doctors Without Borders focuses on emergency, paediatric, and maternal healthcare in Afghanistan, which has one of the highest maternal mortality rates in the world.
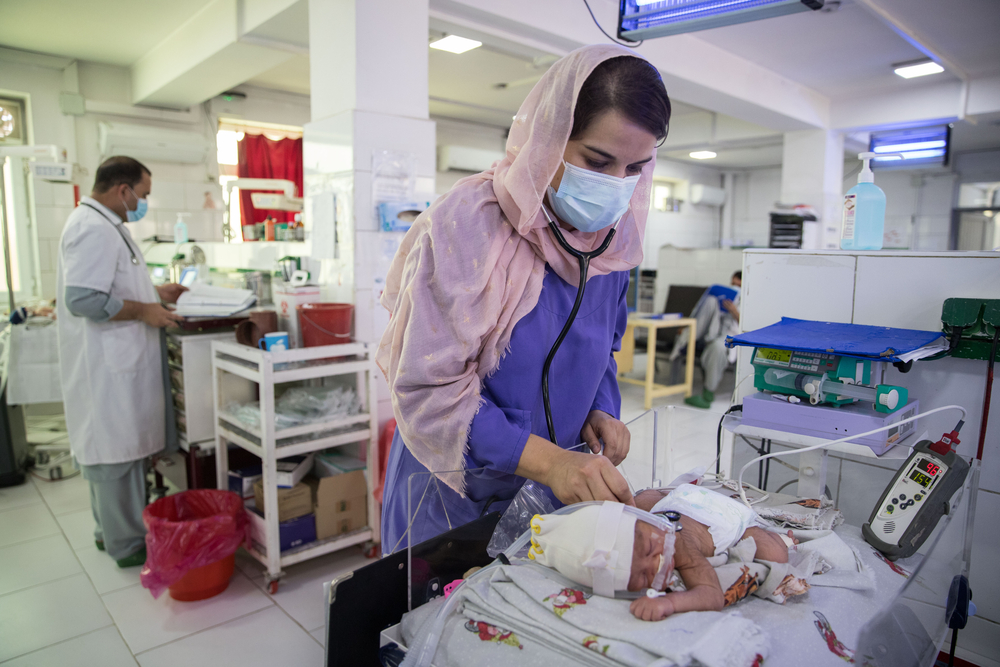
In Helmand and Khost provinces, we provide free, high quality maternal and neonatal healthcare in two hospitals to help reduce death and sickness in mothers and their newborns. Training medical staff is an integral and important part of our projects.
We support the diagnosis and treatment of drug-resistant tuberculosis. In Kandahar province, in the south of the country, we run a laboratory, as well as facilities for hosting patients during their treatment.
In Kunduz, we opened a new 30-bed trauma centre in August 2021. The centre treats people with trauma injuries, for example, as a result of road traffic accidents, and people injured in the fighting who have complications.
In both Herat and Helmand provinces, we treat malnourished children in inpatient therapeutic feeding centres; those coming to the centre at the regional hospital in Herat have often travelled some distance to get there.
In Nigeria, Doctors Without Borders has been responding to disease outbreaks and emergency health needs for many years, focusing on maternal and paediatric healthcare throughout the country. Since mid-2021, we have scaled up our nutritional activities in the Northwest, as a growing yet largely ignored malnutrition crisis is pushing people to the limits.
We support the Noma Children’s Hospital in Sokoto with acute medical care and reconstructive surgery for patients with noma. Most patients with noma ─ a disfiguring and often deadly infection ─ are children under six, whose immune systems have been weakened by malnutrition. In addition to surgery, our team provides physiotherapy, nutritional and mental health support, and conducts outreach activities to improve early detection. In 2021, our staff conducted 105 surgical interventions.

“Noma can be prevented by improving the living conditions of people at risk and raising awareness,” says Karla Bill, Doctors Without Borders health advisor for Nigeria. “And it’s treatable with antibiotics if detected and managed early. But little is known about the disease, and more research and resources are urgently needed to investigate its causes, prevalence and risk factors.”
Access to healthcare remains a challenge in Pakistan, especially for people in rural communities, informal settlements and areas affected by conflict.

In Pakistan, Doctors Without Borders focuses on improving access to healthcare for women and children, and treatment for communicable diseases. In 2021, we also continued to support the COVID-19 response.
At five different locations in Balochistan and Khyber Pakhtunkhwa provinces, we provide reproductive, neonatal and paediatric care services We also assisted local communities, Afghan refugees and people in border areas, running emergency obstetric services and nutrition programmes, and ensuring the treatment and referral of critical trauma patients. We also run a cutaneous leishmaniasis programme, with satellite clinics in Peshawar and Bannu districts.
In Karachi, Sindh province, Doctors Without Borders has a hepatitis C project in the informal settlement of Machar Colony, and started supporting COVID-19 vaccination activities in September 2021.
In Gujranwala, Punjab province, we opened a new project to diagnose and treat people with multidrug-resistant tuberculosis, implementing a decentralised approach, which enables patients to receive care nearer their homes.
This 2022, we are responding to the flood emergency that has affected more than 33 million people across the country, with a death toll that is now estimated at over 1,700.
As the war in Ukraine continues, our teams are responding to a humanitarian crisis. Increasingly urgent requests for medical supplies are coming in from many hospitals and health facilities in the more war-affected parts of Ukraine. Doctors Without Borders is seeking ways to donate what is needed, where it is needed.

Our teams are preparing for a range of scenarios which will allow us to step up our response, including providing surgical care, emergency medicine and mental health support for displaced people. Our current response includes:
- Sending experienced medical staff to Ukraine to support our existing teams;
- Sending new cargo shipments of emergency medical supplies to Ukraine;
- Supporting hospitals and doctors remotely, including via telemedicine;
- Donating medical stocks for emergency surgery and trauma care;
- Preparing warehouses and transport for our supplies;
- Assessing needs in the country and the possibility to reach cities such as Odessa, Mykolaiv or Kherson.